Who is Bili Rubin? Jaundice Explained.
When tiny babies come in to be seen urgently (I’m talking newborns here, like in the first few weeks of life), they get everyone’s attention. Why is this? They’re cute and small, sure, but there are lots of medical reasons as well. There are many germs that hang around sick people, and there’s plenty of those in urgent care offices and emergency departments. Germs and newborns are not a great combination, so we do our best infection control measures when the 5kg crew shows up. We try to have them spend as little time as possible out in the waiting room/reception area in contact with the rest of the sick folks, and we place them in private rooms to avoid picking up anything extra than what they may have already presented with.
But that’s not what I’m really talking about today. That’s what we do regardless of reason for arrival, but perhaps the most common reason the newborn crowd comes in is for jaundice and to get a blood bilirubin level checked. Jaundice. You know: yellow skin. Happens a fair amount to newborns so let’s talk about it real quick.
First, a quick vocab lesson:
Bilirubin is a yellow chemical compound in your body. It’s formed inside your liver by the breakdown of hemoglobin (a protein in your red cells – helps carry oxygen to your cells and tissues)and excreted in bile. When bilirubin is not excreted properly, it builds up in your body, giving your skin that yellowish hue.
The yellow color (which we describe by saying “icteric”-25 cent word!) in the skin and the whites of the eyes (conjunctivae- another 25 cent word!) is due to increased bilirubin, most of which is a breakdown product of hemoglobin in red blood cells. Increased bilirubin deposition can happen for a lot of reasons, from harmless to serious.
The serious ones are really quite rare and most have to do with problems in the liver, and the most common reason is simply a harmless phenomenon of transition from fetal life to being a human in the brand new world. The fetal hemoglobin gets turned into mature hemoglobin, and with that conversion some of that hemoglobin is destroyed, leaving a bunch of bilirubin circulating around. When that happens, hello jaundice.
Why do we care anyway? Because too much bilirubin isn’t great for a developing brain. Not very charming at all. So sometimes we need to help the “getting rid of” process a little bit.
Why Does This Happen?
A few circumstances increase an infant’s risk for getting this accumulation of bilirubin.
Children of East Asian descent, premature and breastfeeding babies are at risk—mostly due to the dehydration that often occurs initially before the mother’s breast milk supply is revving up. It’s as if these babies’ digestive systems just aren’t fully switched on yet, and bilirubin is processed in the abdomen. African American babies are less affected. Babies who have different blood types than their moms can also be what we call a “setup” for jaundice, and low birth weight babies have a higher risk as well.
So once we see the jaundiced color, we get a blood sample to measure the actual bilirubin level. Depending on how many hours/days old the baby is, along with their gestational age in weeks helps us determine whether or not a baby needs phototherapy.
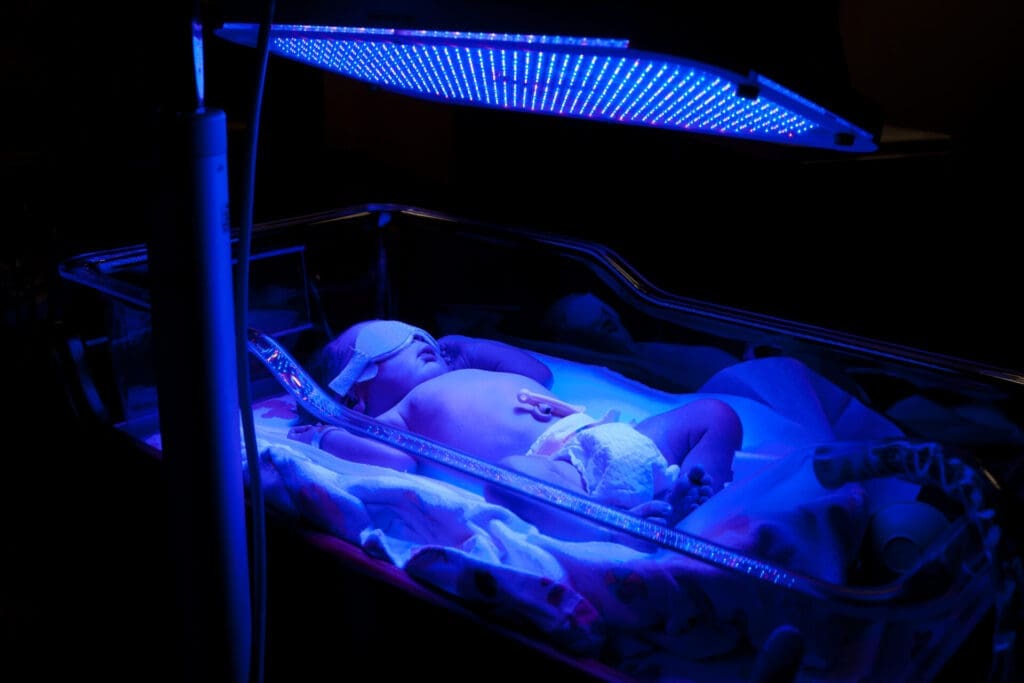
This is the image you typically see with a baby in an isolette under ultraviolet lights with their eyes covered. Some babies just have an ultraviolet light “bili blanket” instead of the full set of lights. The phototherapy gets absorbed through the skin and helps the baby’s body convert the bilirubin to a harmless compound that can be easily excreted through the urine and stool. Serial bilirubin levels are checked until it drops to safe level, and then the whole gig is typically over for good. The best thing for babies during phototherapy is to hydrate and breastfeed LIKE CRAZY! This enhances excretion of that pesky bilirubin.
Is it Jaundice? Symptoms to look out for in infants:
- Yellow skin
- Yellow eyes (scleral icterus)
- Sleepiness
- Poor feeding
- Dark urine
- Fever
- Vomiting
I think that’s enough science for today, but I just wanted you to know a little more about that topic because I see it a fair amount, and I’m guessing you know someone whose baby needed some phototherapy. Finally, I don’t want anyone to be upset if they’re getting acute care for their child and they see a neonate getting whisked in ahead of them. Now you know why.
From strep throat to stitches, we’re here for your family – wherever you are! Click here to find a PM Pediatric Urgent Care near you. Not near to an office? Get care with telemedicine, available in 15 states.
About the Expert

Dr. Christina Johns is a nationally recognized pediatric emergency physician and Senior Medical Advisor at PM Pediatric Care. An official spokesperson for the American Academy of Pediatrics, she is board-certified in both pediatrics and pediatric emergency medicine. With extensive media experience, the proud mom of two teenagers shares over 20 years of pediatric expertise with patients and families everywhere. Follow Dr. Johns for more insights on children’s health!